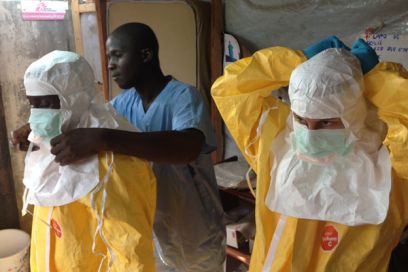
Ebola has already killed over 5,000 people and infected over 400 healthcare workers. Modeling the worst-case scenario, CDC now predicts 1.4 million Ebola cases by 2015. Land spill across contiguous borders in West Africa has created an unprecedented Ebola “hot-zone,” and air travel threatens global spread of disease. This outbreak is one of the largest in history of a viral hemorrhagic virus and the first ever in West Africa. In the United States, the few cases imported have incited irrational fear which is not only unwarranted but actually undermines an appropriate response to the outbreak. By focusing on quarantine, we are ignoring the need for centralized public health systems and training to deal with inevitable cases of Ebola.
Ebola is not spread through air, water, or food, but end-stage sick patients can have over a billion viral particles in a cubic centimeter—or about a fifth of a teaspoon—of blood making contact with bodily fluids highly infectious. By comparison, a patient with untreated HIV has 50,000 to 100,000 particles in a similar quantity of blood, and someone with untreated hepatitis C has 5 million to 20 million particles. At times during illness a patient can lose ten liters of fluid through diarrhea and vomiting. It takes little imagination to understand how infectious a patient could be to a health worker or how body fluids at the time of burial pose huge risks of transmitting the disease. But while the virus can survive on dry surfaces for hours and contaminated wet surfaces for days, it is not a particularly hardy one and can be easily killed by bleach. Past outbreaks have been halted in months by quarantine of infected patients, personal protective equipment for health care workers, and proper burial precautions.
What makes this episode different than previous Ebola outbreaks? First, this epidemic has established itself in densely populated urban West African cities. In the past, Ebola “hot zones” have been rural, isolated, and not heavily populated. But more so, this is an issue of global health disparities and a failure of the international community. The cities impacted by this outbreak are situated in post-conflict settings where the health workforce has been egregiously lacking, because of poor pay and brain drain.
The World Health Organization (WHO) estimates a shortage of 4 million healthcare workers globally. Africa, which has 25 percent of the world’s disease burden, has only 4 percent of the health workforce. The three countries most affected by this epidemic, Guinea, Sierra Leone, and Liberia, also have the greatest disparities between healthcare workers and population. Liberia, where my program, The Yale/Stanford Johnson and Johnson Global Physician Scholars, has partnered with the major teaching hospital for many years, counted only ninety physicians in the last census for a population of over 4 million. Two of their most prominent physicians and the only trained internist in the country, Dr. Abraham Borbor, lost their lives to Ebola along with many dedicated frontline nurses. Healthcare workers have been stretched to the limits.
Second, the WHO’s global response has been embarrassingly late, uncoordinated, fragmented, and decentralized. The WHO was alerted to the cluster of cases in Guinea by March, but did not sound the alarm until August. Why did this happen? Sherry Fink’s analysis in the New York Times pointed to the decimation of the WHO budget to a level more or less equivalent to the budget of a single large hospital in the United States. Moreover, the WHO’s pandemic and epidemic division had been disbanded due to budget cuts and duties redistributed. Many veterans of pandemic control had left as a consequence. When almost 80 percent of the WHO budget depends on outside donors, often those donors’ agendas co-opt WHO’s agenda by earmarking funds for member state projects. Now on high alert, WHO has been frantically playing catch-up when it should have been the first to call the alarm.
Due to this crisis in WHO leadership and the inability of a central public health agency to disseminate uniform messaging of the global risk for the disease, fear has taken over, prompting mandatory quarantine of asymptomatic healthcare workers and journalists returning home to the US, and military-enforced quarantines of neighborhoods in affected countries. These edicts are counterproductive, compounding the difficulty of combating Ebola and reporting responsibly on the efforts to contain the virus.
So what are the solutions to this outbreak and some of the ethical dilemmas they pose?
There has been a lot of talk about ZMapp, the monoclonal cocktail of antibodies to the outside glycoproteins of Ebola, used successfully in a few cases. This drug was developed by inserting Ebola genetic material into modified tobacco mosaic viruses and then introducing the modified virus into tobacco plants to grow so-called “plantibodies.” (An irony that tobacco may finally play a role in health!) Given the slow pace of generating ZMapp and the lack of human testing, one can only speculate ZMapp’s efficacy. Other drugs are now being hastily developed and given phase 1 human safety trials. The WHO, having convened an ethics panel (albeit with no representative from West Africa), has officially commented that compassionate use of drugs can be rolled out without human safety trials during this epidemic.
Ebola vaccines are in the development pipeline. Interestingly, Canada had stockpiled almost 1,000 doses of a vesicular stomatitis Ebola vaccine presumably as a defense for bioterrorism. It was developed almost a decade ago by Thomas Geisbert and colleagues and sat on a shelf due to the lack of interest by Big Pharma in funding human safety trials. Now with the epidemic raging, this vaccine is being tested in humans along with an adenovirus-based Ebola vaccine developed by the National Institutes of Health and Glaxo-Smith-Kline.
But serious ethical questions are raised around who will receive the drugs and vaccines and who will decide on that distribution. The first few doses of ZMapp given out were directly negotiated from the manufacturer by Samaritan Purse, a humanitarian NGO, and used for its white, American volunteers. Later a few doses were released for West African physicians. Distributive justice issues loom large, as do fears of patients being used as “guinea pigs.” Ethicists debate whether informed consent could really be non-coercive when the patient has a highly fatal disease like Ebola. If limited vaccines are available should one immunize the few frontline doctors treating patients or should one immunize nurses and janitors, who have the most direct contact with body fluids? Should limited drug supplies be offered only to healthcare workers or should young patients with families to support be offered drugs? If scarce Ebola drugs or vaccines are to be implemented in the field on a compassionate basis, many think we need to study them in randomized placebo trials for efficacy first.
In actuality, the solution to this Ebola crisis is not drugs, mass quarantine, vaccines, or even airdrops of personal protective gear. The real reasons this outbreak has turned into an epidemic are weak health systems and lack of workforce; any real solution needs to address these structural issues. When one physician or nurse is caring for forty to fifty patients, mistakes happen. WHO’s legally binding International Health Regulations (2005) requires wealthier countries to mobilize financial and technical support to help contain an outbreak such as Ebola, for which the Director General has called an international public health emergency. Yet workforce scale-up has been disturbingly slow. NGOs like Médicins Sans Frontières were not equipped to deal with Ebola, and have been overwhelmed by the outbreak. Workforce volunteers for these NGOs have been slow to mobilize and fearful US hospitals have set up barriers by insisting that their employees taking unpaid leave or vacation time and then return to mandatory 21-day quarantines, often without pay.
Humanitarian relief is often chaotic. Coordinating multiple NGOs with the U.S. military and other national volunteers (such as Cuba) has been problematic. Ebola treatment units are being designed and stocked, and multiple training sessions held, without central guidelines or coordination. This needs to be changed. Along with a colleague at Georgetown, I have proposed the formation of a Global Health Workforce Reserve akin to the U.S. Military Reserves, where physicians and nurses with experience in low-resource settings sign up for a period of time and are ready for coordinated deployment when epidemics and catastrophic events occur. A corps such as this could be centrally managed, either at the UN or WHO, and be scaled up quickly. Periodic, short-term boot camps could be held to maintain training in disaster relief and outbreak response. Given the incredible interest in global health training programs in the past ten years, as documented by the Consortium of Universities for Global Health, finding the volunteers and funding should not be a problem.
Lastly, if one looks at the newly evolved and most dangerous pathogens we have had in the past decades—HIV, SARS, MERS, Nipah virus, even pandemic influenza strains—they all have emerged from animal populations. In the case of Ebola, dramatic gorilla die-off has been well documented six to nine months before human cases. Prevention of Ebola outbreaks by identifying early hot-zones and spillover of disease into human populations could be achieved by the One Health Initiative, which advocates healthy husbandry, attention to conservation, and enhanced biosurveillance of animal disease. Taking this more comprehensive and multidisciplinary approach linking human, animal, and environmental health offers the best chance for a healthier planet.