Nine years ago Rafael Braga was collecting cans to recycle for cash not far from a political demonstration in Rio de Janeiro when he was stopped and arrested by police. A twenty-five-year-old Black man, unhoused at the time, Braga carried two bottles of cleaning detergent in his pocket. Police claimed he carried explosives.
The judge bought it. Braga was convicted of possession of a Molotov cocktail and sentenced to five years in Rio’s Bangu Penitentiary Complex, a maximum security prison. He was the only person to land a prison sentence during the countrywide Revolta do Vinagre, or Vinegar Protests, which rocked the country in 2013 after protesters were arrested for carrying vinegar as a remedy for tear gas used by police. In 2015 Braga was released with an ankle monitor but soon rearrested and charged with drug trafficking after police found him carrying less than a gram of marijuana. Two years later his lawyers announced that his already severe eleven-year sentence for the trafficking charge had been effectively increased: like more than 10,000 other incarcerated Brazilians that year, Braga had been diagnosed with tuberculosis (TB).
Braga’s story highlights the insidious and growing role prisons play in fueling another devastating pandemic most of the Global North has all but forgotten. Before SARS-CoV-2 spilled over into humans, TB claimed more lives worldwide than any other infectious disease. In 2019 alone, 1.4 million people died of the illness—more than twice the number who succumbed to HIV/AIDS—while some 10 million people fell ill, all of whom require a grueling six-month treatment regimen of antibiotics that often come with intense side effects. The COVID-19 pandemic has only made things worse. For the first time since 2005, the global TB death toll increased in 2020, a result of widespread disruptions in access to essential health care, leaving millions more people undiagnosed and without treatment. As these missed cases transmit infection in turn, the effects of COVID-19 on global TB cases and deaths are predicted to escalate in the coming years.
Despite this incredible toll, we in the United States hardly ever hear about the steady stream of people who fall victim to this forgotten pandemic. There is no New York Times world map for TB, no daily mass media surveillance of global case and death counts—no mechanism, that is, to fuel popular outrage or even awareness of so much needless and preventable death. As with many global health crises, from the extreme weather accompanying climate change to the rapid spread of drug-resistant bacteria, the impact of TB falls overwhelmingly on the poor and non-white. And as Braga’s case makes clear, reckoning with its burden today requires facing how the disease is perpetuated by institutionalized racism, global capitalism, and mass incarceration.
When I began studying TB four years ago, more than one friend expressed surprise. Hadn’t the disease been more or less eradicated? The question exemplifies the West’s historical amnesia when it comes to infectious disease.
TB’s roots are ancient. More than two millennia before modern science identified the bacterial culprit, Hippocrates wrote of the horrors of phthisis, as the malady used to be called—literally, a “wasting away.” TB was the leading cause of death in industrialized countries until the mid-nineteenth century, and popular representations still portray it as a bygone affliction of European bohemians and elites. “Chopin coughs with infinite grace,” wrote the novelist George Sand about her lover, who likely died of the disease.
The twentieth century saw the development of important treatments and controls, from vaccines to antibiotics, but these resources have never been distributed equitably. “The advent of effective therapy seems only to have further entrenched this striking variation in disease distribution and outcomes,” the late physician-anthropologist Paul Farmer wrote. And the disease continues to decimate global populations and mutate into dangerous antibiotic-resistant forms. “TB kills the equivalent of one Boeing 737 plane crash every ninety minutes,” Tom Scriba, director of the South African TB Vaccine Initiative, reminded the audience at a recent lecture.
Why does this ancient disease endure? One reason is that the tools we have to prevent and treat disease are shamefully outdated and unequally distributed. For one thing, vaccine apartheid reigns. In the case of COVID-19, vaccines are hoarded by wealthy countries; in the case of TB, reliable vaccines do not even exist: the only one in common use is the bacillus Calmette-Guérin (BCG) vaccine, which is more than a century old and often ineffective at preventing the most common forms of adult disease. Excruciating treatment regimens have also gone largely unchanged for decades; developing a new TB vaccine or antibiotic is not a lucrative move for a pharmaceutical company. And public health programs including TB control are chronically underfunded, meaning that the treatments that do exist are prohibitively expensive and a loved one’s TB diagnosis remains a “catastrophic cost” in many countries. Millions more people with TB are not diagnosed at all.
The distribution of biomedical interventions alone, though, cannot explain TB’s ugly persistence. Historians argue that more general improvements in living and working conditions and better nutrition dramatically decreased risk of TB in Europe and North America well before the widespread use of antibiotics. But billions of people are still forced to live and work where TB remains endemic.
According to the World Health Organization, roughly two-thirds of new cases are concentrated in eight countries: India, China, Indonesia, the Philippines, Pakistan, Nigeria, Bangladesh, and South Africa. Among other high-burden countries are the Democratic Republic of the Congo and Mozambique, two of the poorest nations in the world. In Ukraine, continuous war and displacement has fostered the uncontrolled spread of multi-drug resistant TB even before the current Russian invasion, and many fear that the ongoing refugee crisis will trigger wider epidemics across Europe.
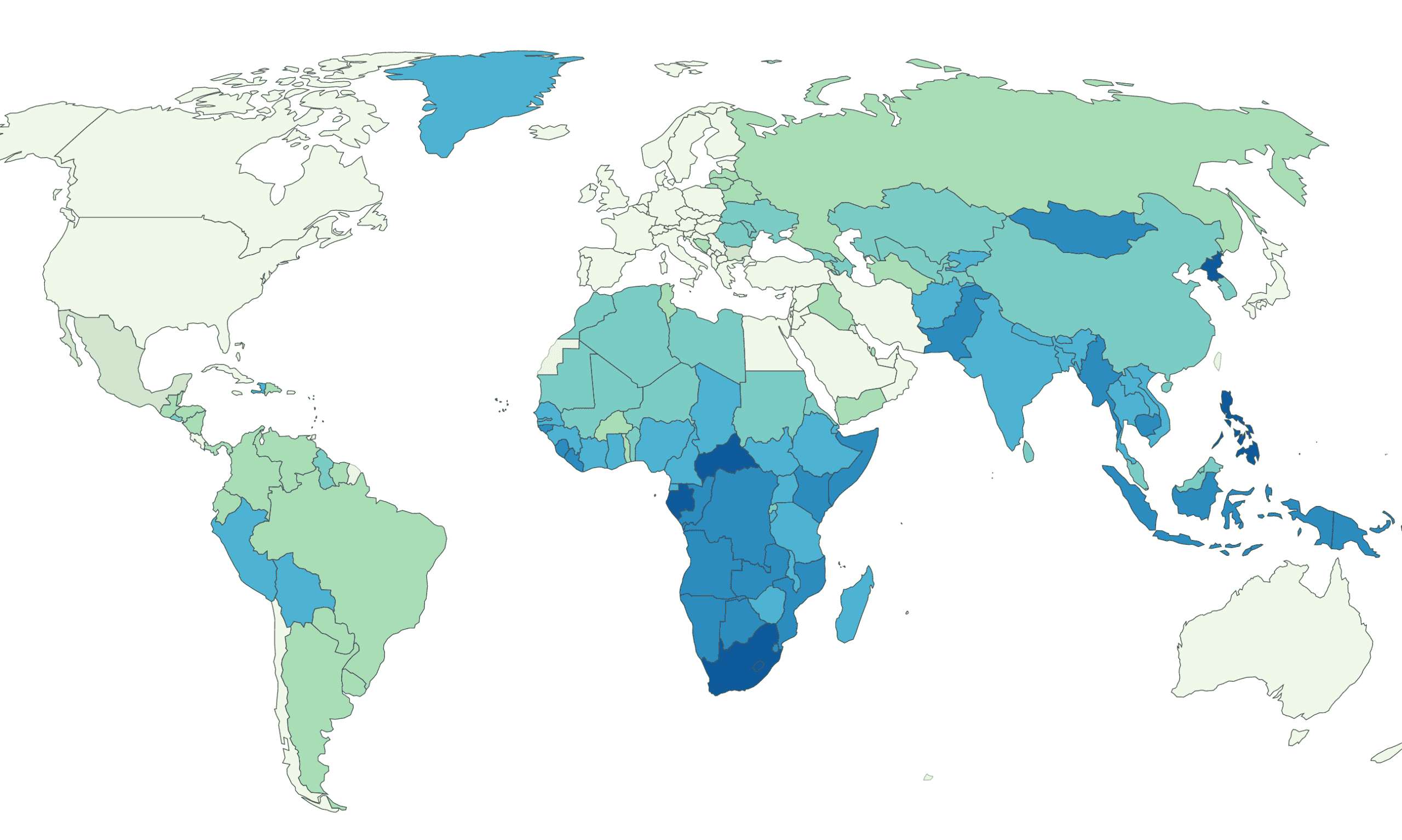
No matter where we look, the same pattern emerges: the burden of TB falls along lines of race, class, and social vulnerability. Through the early twentieth century, the disease devastated Native populations across North America and globally, indigenous peoples continue to bear a higher rate of TB than do surrounding populations. By 2019 the U.S. incidence of TB was the lowest reported since reporting began in 1953, but progress against the disease has not been distributed equally. Though the majority of TB cases in the United States occur among people born elsewhere, among people born here Black people are nearly seven times as likely to have TB as white people. Moreover, in 2020, 3 percent of all TB in the United States occurred among incarcerated people—about four times the rate you would expect based solely on population demographics (incarcerated people accounting for about 0.7 percent of the population). And in 2020, 327 people were diagnosed with TB in ICE custody.
As Braga’s case illustrates, these patterns also extend to Brazil. Over the last 20 years, Brazil’s prison population has more than tripled, increasing from 232,755 in 2000 to 759,518 in 2021. The country now holds the third largest incarcerated population in the world, trailing only China and the United States. And while the incarceration rate in the United States peaked in 2008, Brazil’s incarceration rate continues to climb under the right-wing President Jair Bolsonaro. “I’ve always said it,” Bolsonaro tweeted during his 2018 election campaign: “I prefer a prison full of criminals than a cemetery full of innocents. If space is missing, we build more!”
Much of the spike in incarceration can be attributed to Brazil’s 2006 drug law, Lucas Sada, Braga’s lawyer and a public defender at the Institute of Human Rights Defenders, told me. The law was a political compromise gone wrong. Though intended to reduce drug-related sentences, in practice it opened the door to separate punishments for drug users and drug traffickers. In 2005, 9 percent of those in prison across the country faced drug charges. By 2019 the figure had skyrocketed to 41 percent.
As in the United States, incarceration disproportionately targets people of color and the poor. According to Brazil’s National Department of Prisons, Black and mixed-race Brazilians made up 66 percent of the incarcerated population but only 53 percent of the national population in 2019. In 2016 most people in Brazil’s prisons had not completed elementary school. And escalating incarceration rates have been paralleled by a tripling of TB cases among incarcerated people from 2007 to 2018. Nationally, 11 percent of all Brazilian cases now occur among incarcerated people, who make up less than 1 percent of the population, and a third of all cases among men Braga’s age—18- to 25-year-olds, the group incarcerated at the highest rate—now occur among the incarcerated. Who gets sent to prison plays a large part in determining who gets sick with TB.
On a warm September morning in 2018 I followed Andrea Santos, a nurse and epidemiologist at the Universidade Federal da Grande Dourados, down a dirt path in Campo Grande in the central western Brazilian state of Mato Grosso do Sul, which borders Paraguay and Bolivia. Here the incarceration rate has more than doubled over the past twenty years, and the majority of those incarcerated are serving time for drug-related crimes. As we walked, a line was forming at the entrance of Estabelecimento Penal Jair Ferreira de Carvalho, a maximum security men’s prison locally known as “Máxima.”
The year before, I had joined Santos and a team, led by the physician-epidemiologists Julio Croda and Jason Andrews, studying Brazil’s increasing TB epidemic. While prisons were known incubators of TB, there was a dearth of evidence about how to actually reduce TB inside, Andrews told me. He and Croda sought a way to find cases and treat them early, before infection could spread. In Brazil they were piloting mass screening approaches involving routine testing of the entire prison that the World Health Organization had dismissed as too expensive “in resource-limited settings.”
Santos was part of this effort, and she wanted to show me her work collecting sputum—phlegm coughed up from the lungs—to screen for TB in Máxima, but on our drive over she was visibly worried. Some Mondays, she said, the entire prison was locked down after weekend clashes between guards and prisoners, and even health care workers weren’t let in.
This Monday, Máxima was open. The air inside was stagnant. We passed a cell filled with a few dozen men who sat on bunks three levels high, ankles dangling near faces, laughter and smoke filling the cell. If one of them were sick with TB, the infection would likely spread fast. As with SARS-CoV-2, Mycobacterium tuberculosis transmission is airborne: once exhaled from someone’s mouth, the bacteria can hang in the air for hours, suspended inside tiny particles called droplet nuclei. As the COVID-19 pandemic has made all too clear, airborne pathogens are particularly devastating in congregate settings.
In 2013 Juliana Urrego, an architect-turned-epidemiologist in Andrews and Croda’s group, surveyed the architectural risk of a prison sentence in Mato Grosso do Sul. Extreme overcrowding is the rule, she found. People are locked in more than eight to a cell for more than eighteen hours a day. On average each person is allotted two square meters of space, about the footprint of a standard bathtub, and cement bunks are in short supply. Some men share a bunk, sleeping head-to-toe, Santos told me; others had the floor. Little of Mato Grosso do Sul’s searing sunlight filters into cells, limiting the UV radiation that can inactivate M. tuberculosis. Urrego’s team installed carbon dioxide monitors in 141 cells to track the flow of exhaled breath and the potential risk of TB transmission. Unsurprisingly, the air was stagnant. With a model of TB transmission, Urrego found that breathing and re-breathing the same air carried a weighty epidemiological risk: six months of sharing a cell with a single sick cellmate would result in a 79 percent risk of TB infection.
Prison practices only further compound transmission risk. Everton Lemos, an infectious disease nurse in the group, digitized cell-level movements within the state’s prison registry to determine how infection risk spread within prisons. Guards moved people between cells eight or more times a year, he found—adding up to more than sixty cell contacts, each a new potential exposure, each year. Poor-quality prison food, along with a heightened risk of infection with HIV or other pathogens, also increases TB susceptibility. All the while, a shortage of doctors or diagnostic tools, including X-ray machines and equipment for molecular diagnostic tests, means that if someone gets sick, there is often a substantial delay before they are diagnosed, if they are lucky enough to diagnosed at all. Each day someone goes undiagnosed is a day they could potentially infect others.
Next to the door Santos and I entered was Máxima’s other entrance, which whined open several times a day for trucks full of supplies and armed prison vans shuttling staff, guards, and men in handcuffs. Santos estimated several hundred visitors moved in and out of the prison each Sunday alone. This porousness of prison walls underpins a second, more self-interested, argument for controlling the epidemic inside prisons: bacteria do not heed locked doors. As Andrews pointed out to me, the New York Times made the same hollow argument as far back as 1903: “If the prisoners are not properly the objects of sympathy, perhaps the people outside the prisons may be so considered.”
In one study led by Tarub Mabud, then a medical student in our group, our team tracked TB cases among people who were cycled through the prisons in the state. When people are first incarcerated, they are infected with TB at about the same rate as the population outside prisons. With each year of incarceration, however, TB incidence rises dramatically to a rate 31 times that of the unincarcerated population. The mass screenings led by Santos revealed an even grimmer picture than had been captured by the state’s passive surveillance. By testing each incarcerated individual every six months, the group found that incidence of TB in Máxima and other prisons in the state is over 5 percent, a rate that Andrews called “among the highest” ever reported in the world—evidence that current data likely grossly underestimates the true burden of the disease in prisons. Prison itself thus determines this excess risk of disease, not—as some critics retort—a characteristic of the people who are sent there. And the epidemiological shadow of the prison is long. For seven years following someone’s release, their risk of developing TB—and of transmitting it to the families and communities they’ve returned to—remains many times higher than general risk in the community.
Epidemiologists consider prisons like Máxima institutional amplifiers, reservoirs of fuel that keep the epidemic burning. Brazil is hardly unique. Studies in Russia, Brazil, and many countries report that one of the greatest risk factors for TB is previous incarceration or contact with someone who has been incarcerated. At the same time, TB propagation beyond prison walls has been difficult to measure. Latent infection often lingers undetected, causing no symptoms for months or even years before people develop symptoms and can then transmit the bacteria to someone else. It’s thus very difficult to say with high confidence precisely where and when someone was infected, at least using traditional epidemiological tracing. The bacteria themselves, though, hold their own record. As M. tuberculosis copies itself during an infection, the bacterium’s replication machinery occasionally makes errors. By sequencing the M. tuberculosis genome and tracking these mutations, we can puzzle out likely chains of who-infected-whom, revealing sources of infection.
Andrews and Croda’s team carefully incubated sputum samples for weeks until a deadly topography emerged—what looks like clumps of white fish eggs rose from a sea green medium. By sequencing more than 1,000 of these bacterial cultures from people inside and outside prisons, we reconstructed a partial picture of transmission in Mato Grosso do Sul. Bacterial genomes formed tightly related clusters, indicating that transmission had occurred very recently. Transmission clusters often spanned prisons and surrounding communities. So-called “spillover events,” transmission from prisons to communities outside, occurred in many cities across the state. People are moved frequently, between prisons and between prison cells, creating a highly connected contact network and ample opportunities for disseminating M. tuberculosis into new, highly vulnerable populations across the state. Prisons are not only reservoirs of disease, in other words, but serve as epidemic pumps, distributing the risk of disease far beyond prison perimeters.
If prisons play an outsized role in perpetuating the TB epidemic in Brazil, Andrews and Croda hypothesized, public health interventions should be focused there. Mabud used epidemic models to forecast the effect of an approach combining frequent TB screenings with isoniazid preventive therapy treatment of patients discovered to have latent TB. Within ten years, our group estimated, incidence of TB would drop by 80 percent inside prisons and 40 percent outside.
But the most effective intervention of all, of course, is beyond the realm of traditional public health approaches. “First of all, very importantly, we need to reduce the number of people who are jailed, detained and in prison all together,” Chris Beyrer, epidemiologist and human rights scholar at Johns Hopkins University, told me in an interview in 2017. “Prison is a very bad place for anybody to be.” One place to start is the war on drugs, Beyrer said. “People who use drugs don’t need to be there. We need to decriminalize the possession and use of drugs.”
Another place to focus is decarceration. Releasing people from prison, it turns out, is not a new epidemiological intervention. In 1999, in the face of uncontrolled transmission of multi-drug resistant TB in prisons, Russia granted mass amnesty, allowing thousands of people to return home early. The COVID-19 pandemic, for its part, has also helped shine a light on the public health risks of mass incarceration, both to those imprisoned and to our communities at large. In 2020 the U.S. National Academies of Science, Engineering, and Medicine assembled experts in law, medicine, and public health to recommend strategies to reduce the exorbitantly high risk of COVID-19 in prisons. “Decarceration is an appropriate and necessary mitigation strategy to include in the COVID-19 response in correctional facilities,” they found.
Some targeted releases have been made in the United States in this direction, but unsurprisingly, they have tended to disproportionately benefit white people. In a paper uploaded in January to the medRxiv (a repository of research preprints that have not yet undergone peer review), a group of researchers at Yale and Northeastern found that, as a result of these releases, the proportion of Black and other non-white incarcerated people rose sharply in 2020. “One of the most important consequences of bias in releases is not only about who is released, but who is left behind,” the authors write. The American Public Health Association, for its part, argues for nothing less than the “abolition of carceral systems and building in their stead just and equitable structures that advance the public’s health.”
Unfortunately, there is little current momentum for decarceration or abolition as an element of TB control. In its annual global TB report, the WHO does not list incarceration as a risk factor, despite the fact that across the Americas what epidemiologists call the “population attributable fraction” of incarceration exceeds that of smoking, alcohol use, diabetes, and HIV. Nor does the WHO publish statistics on the number of incarcerated people who contract TB each year. This fixation on individual risk factors obscures the institutions and places that make people sick. As physician and activist Rupa Marya has observed, “Social/environmental issues are more predictive than genetics for the majority of diseases we treat in medicine—so why do we ignore them? Because medicine is a colonial entity. By focusing on individuals, we continue to hide where the real pathology lies.”
Braga’s case was one of “the greatest symbols of the class and racist selectivity of the Brazilian criminal justice system in the last decade,” Sada, Braga’s lawyer, told me. Soon after Braga’s arrest in 2013, and through his illness in 2017, an activist group, Pela Liberdade de Rafael Braga Vieira, protested and mounted a campaign on social media, making his story famous across Brazil and reported upon internationally.
On September 12, 2017, their collective work led to a small victory. Brazil’s Superior Court of Justice would allow Braga to move to house arrest for his recovery from TB. “The grotesque picture of violations of fundamental rights,” the court wrote,
reaches a different level in cases that, like that of Rafael Braga Vieira, deal with individuals who meet the common profile of those incarcerated in the country: Black people, young people, with low income and schooling who, inside prisons, continue to suffer the hardships of the state’s lack of interest in providing, with a minimum of quality, public services which, even for those deprived of their liberty, cannot be denied.
At the same time, the court continued, its ruling “does not imply recognition that any and every person imprisoned, sick, in a prison in this country has the right to house arrest.” The decision brings no relief to thousands of others, unnamed by the press, who fall sick each year.
Prison abolitionist Angela Davis has argued that “prisons do not disappear problems, they disappear human beings.” TB is a case in point. Behind prison walls, in detention centers and urban slums, people are abandoned by health systems, by mainstream media, by social services essential for living a healthy life. “At their worst,” historians of medicine Jeremy Greene and Dora Vargha recently wrote in these pages, “epidemic endings are a form of collective amnesia, transmuting the disease that remains into merely someone else’s problem.” TB endures in large part because the people at greatest risk have been rendered invisible, and it up to us to insist, as Farmer did, “that no one should die of tuberculosis today.”
Boston Review is nonprofit and relies on reader funding. To support work like this, please donate here.









