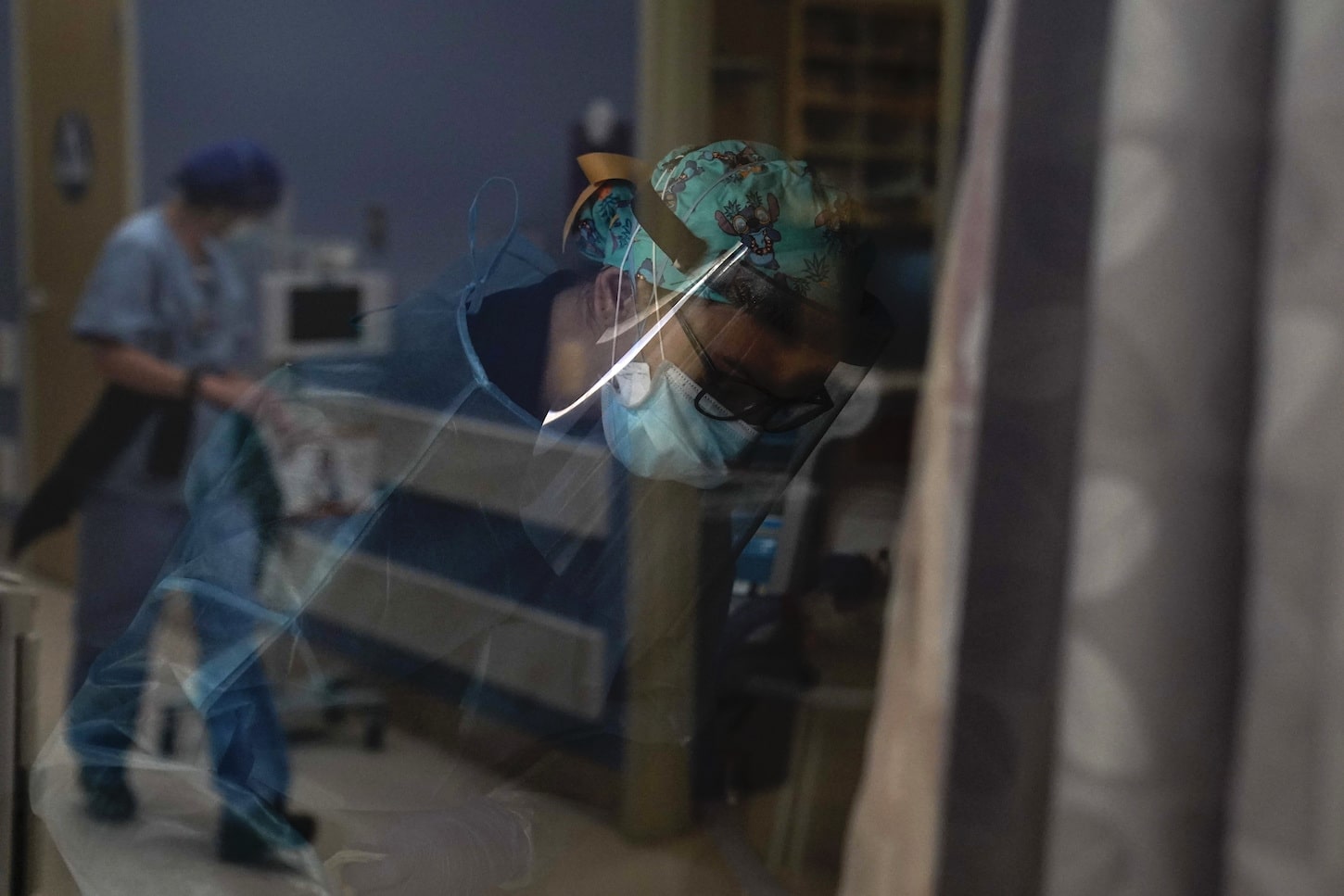
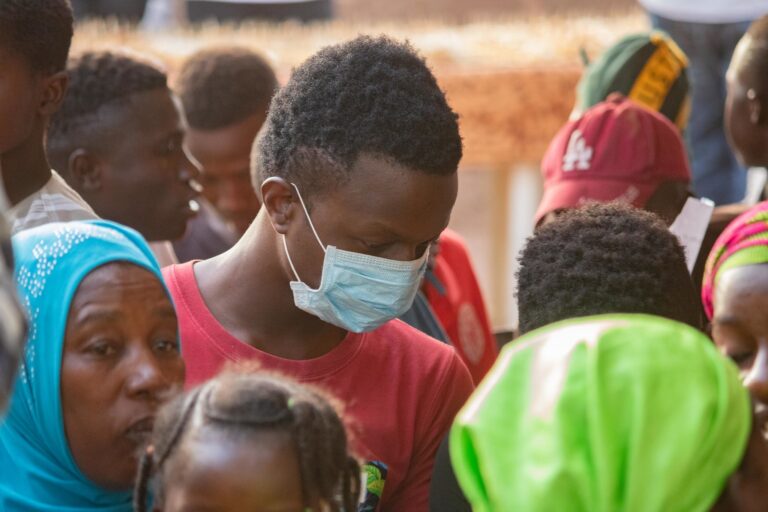
This forum appears in print in Uncertainty.
The COVID-19 pandemic has confounded the world’s expectations at every turn. It began in surprise, continued with chaos, and devolved into conspiracy theories. From a policy standpoint, it gave the lie to our prepandemic imaginations of order and control. Public health experts, after all, had warned of an outbreak for decades. But despite its prominence among the grand global challenges that successive U.S. presidents were advised to take seriously, it still caught this nation and many others flatfooted. Nineteen months into the pandemic and counting, the balance sheet of losses and gains in the United States leans negative across public health, the economy, and democratic politics. How can we begin to make sense of a widely predicted crisis that, by late October 2021, had carried off nearly 5 million lives worldwide, stalled economies, and placed unprecedented strains on social ties and personal liberty?
The mistake, I argue, was to overestimate the certainty of our predictions and our capacity for control. Prediction as a policy tool focuses on identifying chains of causation and assessing their likelihood before bad things happen. That approach has scored great successes, most notably in alerting the world to the threat of climate change well before droughts, wildfires, and record-breaking storms showed ordinary people that weather was turning calamitous. Prediction, however, also falters under the weight of its own ambitions. Disasters happen, and hindsight often reveals overconfidence in the pictures of nature and society on which predictions were based. The makers of thalidomide and diethylstilbestrol did not test for side effects on children born to pregnant women. NASA launched the Challenger without fully analyzing data on the performance of the rocket’s O-ring seals at unusually cold temperatures. Promoters of biofuels failed to calculate the effects of incentivizing these crops on the production of essential food grains. The Fukushima Daiichi planners did not count on a 9.0-magnitude earthquake or a fifteen-meter tsunami at the site of the nuclear power plant.
To counter prediction’s problems of complexity, ignorance, and uncertainty, the policy world recommends precaution. Commonly traced to German environmental policy of the early 1970s, the precautionary principle—or Vorsorgeprinzip—instructs public authorities to plan ahead and act to prevent serious harm to humans and the environment even in the absence of full scientific certainty. This principle has been widely adopted in international agreements such as the 1992 Rio Declaration on Environment and Development and the European Union’s Maastricht Treaty of the same year. Yet precaution remains deeply controversial. Critics frequently dismiss it as a recipe for inaction and stagnation. A notable U.S. example is Cass Sunstein’s scathing denunciation of Europe’s reliance on precaution as fear-driven, paralyzing, and self-blinding.
Advocates of precaution insist that the principle does not stand for passivity or resignation. It was developed precisely to enable and justify prudent forward movement to serve the common good, even when the consequences of acting cannot be completely known. Still, an asymmetry remains that works in favor of prediction and discourages precaution. It is easy to assert our calculative power and deploy our technologies, but less easy to say when to hold back or how not to act. Can one operationalize the precautionary mindset as a positive alternative to the known failures of prediction?
What I offer here is a plea for humility, not merely as a stance of modesty vis-à-vis the powerful and still poorly understood forces of nature and society, but also as a practice of reasoning and policy that accepts uncertainty as its foundation and harm mitigation as its goal. If we mean to do better against the inevitable next time, how should we diagnose what went wrong in the preparations the world had for so long been cultivating, and how should we plan more effectively for the next crisis that will surely come?
The answer cannot be simply to embrace a policy of preparedness toward every possible hazard. To be prepared is a stance of courage and conviction. It implies not merely that one is ready for all contingencies, but that one is confident of one’s ability to meet and overcome them. Britain’s Robert Baden-Powell, who founded the Boy Scouts and chose their motto “Be Prepared,” explained that it meant one should be ready “for any old thing.” The United States Coast Guard glosses its motto—semper paratus (always ready)—to mean that all of its resources are available to meet the nation’s needs and to play “an integral role in mission execution.” Preparedness, in short, is a heroic, can-do posture, bravely denying the possibility of defeat.
Humility, by contrast, admits that defeat is possible. It occupies the nebulous zone between preparedness and precaution by asking a moral question: not what we can achieve with what we have, but how we should act given that we cannot know the full consequences of our actions. Thought of in this way, humility addresses the questions perennially raised by critics of precaution and refutes the charges of passivity. Confronted on many fronts by riddles too knotty to solve, must society choose either to do nothing or to move aggressively forward as if risks don’t matter and resources are limitless? Decades of effort to protect human health and the environment suggest that the choice is not so stark or binary.
There is a middle way, the way of humility, that permits steps to be taken here and now in order to forestall worst-case scenarios later. It implements precaution by unheroic but also more ethical means, through what I call technologies of humility: institutional mechanisms—including greater citizen participation—for incorporating memory, experience, and concerns for justice into our schemes of governance and public policy. This is a proactive, historically informed, and analytically robust method that asks not just what we can do but who might get hurt, what happened when we tried before, whose perceptions were systematically ignored, and what protections are in place if we again guess wrong.
An Anatomy of Preparedness
Since 1945, when the Los Alamos physicists got their first taste of science as sin, the United States has been preparing for catastrophic events that place the nation’s health, security, and identity at extreme risk. Indeed, the shock of catastrophe came even earlier, at Pearl Harbor in 1941, when the U.S. government failed to read the tea leaves of Japan’s military ambitions in time to stave off a devastating attack on U.S. soil. Nor did the surprises stop with the war’s end. Every major U.S. crisis since World War II—the Cuban Missile Crisis, defeat in Vietnam, Three Mile Island, 9/11, the Great Recession, COVID-19, and the rapid fall of Kabul to the Taliban—has generated the same dynamics of self-questioning. Why did we not know when the information was there to be known? Why were we caught unprepared?
The short answer is that we embraced preparedness when we should have opted for precaution. We invested mainly in the arts of control when instead we might have chosen the ethos of responsibility. The pandemic offers an especially illuminating case on which to hang this argument. In some sense this was the most expected of all unexpected events. To borrow UK prime minister Boris Johnson’s poignant phrase about the sudden surrender of Afghanistan, COVID-19 was the “chronicle of an event foretold.” Since the Great Spanish Flu of 1918–1920 took more lives than fighting did in World War I, we have known that deadly respiratory illness can spread around the world with great speed and ruinous impact. Variants from that century-old pandemic still plague the world in the form of seasonal influenza viruses that cause hundreds of thousands of deaths each year. Since then, rising populations, closer contact between people and virus-incubating animals such as birds and bats, and above all the growing mobility of human populations have amply set the stage for recurrent pandemics.
There were many early warnings before COVID-19. In 1994 science writer Laurie Garrett shocked the American reading public with her best-selling book The Coming Plague, which warned of rampant epidemics in a “world out of balance.” Widely praised for its dense coverage of the epidemiology of past infectious disease outbreaks, Garrett’s book gloomily concluded that in the long standoff between humans and microbes, “the microbes were winning.” The years before and since offered many examples on scales that should have caused people to worry, and worry they did. AIDS appeared in 1981 and, though infections and deaths peaked in 1995, forty years of the disease claimed roughly as many U.S. lives as eighteen months of COVID-19. Other viral disease epidemics with transnational spread occurred at frequent intervals: SARS-CoV-1 in 2003, MERS-CoV in 2012, and Ebola in 2014.
Even popular culture did its bit to raise awareness. In an example of life following art, former UK health secretary Matt Hancock told the BBC in February 2021 that the 2011 film Contagion had taught him the importance of having enough vaccine supply for the entire population and being clear about the order of priority. In fact, after badly fumbling the first phases of the pandemic, Britain was widely acclaimed for its vaccine rollout, “the front line in what has become the most ambitious peacetime mass mobilization in modern British history.”
Public and private risk assessors strove for years to prepare responsibly for the great plague that all were sure would come. Possibly the most visible international effort, the Global Health Security Index (GHSI), came about in response to the Ebola epidemic as a joint project among three expert bodies with deep knowledge of risk: the Nuclear Threat Initiative, the Johns Hopkins Center for Health Security, and the Economist Intelligence Unit. The 2019 GHSI provided a preparedness snapshot for each of the 195 parties to the International Health Regulations. Billing itself as the most comprehensive benchmarking of nations’ capacity to deal with infectious disease outbreaks, the GHSI organized its findings under 6 categories, 34 indicators, and 140 questions. Unsurprisingly perhaps, the United States and the United Kingdom scored highest while small, war-torn, and politically unstable states fared worst, with North Korea, Somalia, and Equatorial Guinea bringing up the rear in national capacity.
Meanwhile, public health experts in the United States and elsewhere mined historical outbreaks to construct game plans for future epidemics. The Obama administration left its successor a detailed Playbook for Early Response to High-Consequence Emerging Infectious Disease Threats and Biological Incidents. The document divided the risk world into two rubrics: one for an international response geared toward outbreaks anywhere in the world, with Ebola as its model, and the other for a domestic response to address disease outbreaks within the United States. A key recommendation was to create a “dashboard” signaling the severity of the threat, from green for normal operations to deep red once a threat was established. The playbook, like the GHSI, proposed categories and indicators to assess the risks involved, though its framework showed greater awareness that epidemics are social as well as biological events. For instance, the playbook flagged humanitarian impacts, political stability, and public concern as relevant dimensions of risk. It was a valiant attempt to identify all the relevant questions that should be asked at the onset of an outbreak, compiled with the earnest attention that one might expect in a first-rate “policy analysis exercise” at one of our top public policy schools.
A third document to set beside the GHSI and the playbook appeared early in the pandemic, on April 1, 2020. This was an editorial in the New England Journal of Medicine titled “Ten Weeks to Crush the Curve.” The author, Harvey Fineberg, is one of the nation’s foremost public health experts, former provost and dean of public health at Harvard, former president of what is now the National Academy of Medicine, and chair since March 2020 of the Standing Committee on Emerging Infectious Diseases and twenty-first-century Century Health Threats. With stringent public health measures already in place, Fineberg’s editorial was not so much a guide to preparedness as a manifesto on how to respond when the walls against infection have already been breached. From its first sentence, the editorial adopted President Donald J. Trump’s framing of the problem as a declaration of war. Fineberg’s six-step program, pitched as a call to arms, aimed to bring the virus under control and set the economy back on track by June 6, 2020, the anniversary of D-Day. Step one was to “establish unified command.”
All three documents—the GHSI, the playbook, and the Fineberg editorial—earn high marks as delineations of steps that intelligent and decisive policymakers should take in their efforts to be prepared for emerging infectious diseases. But how do these well-defined preparations hold up against a world in which the unexpected is the order of the day? In spite of their disparate origins and different purposes, two things can be said about these three efforts. It is clear in retrospect that none of the authors paid much attention to the swiftly moving, shape-shifting events, cutting across geopolitical lines, that impede rational analysis and effective response during an actual pandemic. This is partly because all emerged from a militaristic mindset, in which the goal was clear, public buy-in was presumed, and challenges were seen as more logistic than political—more a matter of mobilizing resources, as the Coast Guard pledges to do, than of exploring how to generate the will to act or the risks, costs, and distributive impact of wrong decisions.
The Unraveling
Fast forward to October 2021. According to the Johns Hopkins Coronavirus Research Center, the United States, which led the GHSI as top scorer in preparedness, has the highest number of recorded COVID-19 deaths in the world, a staggering 740,000. The UK, ranked number two in the GHSI, has recorded more total deaths than any EU country. More tellingly, Britain ranks ahead of most major EU countries in deaths per 100,000 population. By contrast Germany, placed at 14 in the GHSI, ranks 22 in the number of deaths per million in the European Economic Area plus Britain, well below the UK in tenth place. Clearly, preparedness and performance were not perfectly aligned. As one influential team of observers concluded, there was an “extreme discrepancy between expected and actual performance for most countries.”
And what of the playbook’s impact on the U.S. response to COVID-19? None was detectable, and its very existence proved to be a point of controversy. In May 2020 Senator Mitch McConnell criticized the Obama administration for not leaving any guidance on a possible pandemic, falsely claiming that its experts had miscalculated the threat as a rare, once-in-a-century event. PBS reviewed the evidence and found McConnell’s assertion blatantly untrue. Interestingly, however, the PBS assessment left open the question of the playbook’s relevance: “whether the Obama plan was dated because it dealt with lessons learned from earlier outbreaks that may not apply to the current pandemic.” Datedness, however, was not the playbook’s most important problem: it was overconfidence in the nation’s willingness to set aside politics and act in unison for the common good.
As to Fineberg’s plan for all-out mobilization, June 6, 2020, came and went, and so did June 6, 2021. Instead of crushing the curve, in late summer of 2021 the United States entered a new phase of dangerously rising caseloads as the Delta variant created a map of intensified infection. The virus that should have been conquered a year back according to Fineberg’s script was no longer quite the same virus. Nor had U.S. governance ever involved the centralized control that the nation’s leading public health experts yearned for. Mask mandates crystallized the conflict and turmoil that still surround efforts to fight the novel coronavirus. The return of indoor masking even in well-vaccinated cities such as Boston spelled one kind of defeat. The microbes were gaining the upper hand again. In less excusable confrontations, the governors of Florida and Texas went to war against their own cities and school districts to prevent masking orders for students from taking effect—not exactly a picture of efficient, centralized high command in action. And the tarnish of breakthrough infections and vaccine hesitancy partly dimmed even the luster of savior vaccines developed, approved, and rolled out at breakneck speed.
A Diagnostic Moment
COVID-19’s disastrous progress around the world brought to light something we had conveniently forgotten, or sidelined, over many decades of success in global efforts to understand and combat human disease: to a greater or lesser extent, securing public health and public safety requires human beings to give up aspects of their liberty in the interests of a common good. Building the regime of public health sovereignty is thus a profoundly political project, not simply a matter of technical knowledge and logistics. We may make those sacrifices willingly, in the name of science and communal benefit, but there are limits and it takes a special kind of work for governments to hold on to people’s allegiance even in times of crisis.
To what extent did the advocates of preparedness take the politics of public health into account? All were aware of possible political constraints, but the specifics of that awareness took different forms, reflecting different appraisals of public health institutions’ authority and expertise. At one pole we have Fineberg’s call for total national wartime mobilization to crush the curve. To be sure, this was to be a democratic process. The fifth step in his six-point program was for the nation’s leadership to “inspire and mobilize the public.” But the actions Fineberg called for to inspire and mobilize presupposed United States that never was, or had long since ceased to be.
In particular, Fineberg imagined a United States in which a respected Postal Service would join with “willing private companies” to deliver hand sanitizer and surgical masks to every door. In reality, the early months of the epidemic saw everyone scrambling and hoarding to get access to such essentials as hand sanitizer and toilet paper, because supply chains failed and stores were entirely out of it. A colleague of mine won Zoom ovations from others at a faculty meeting because she had impressed her aged mother, teen-age children, and husband into making masks at home, a shining example of U.S. individualism rising to the challenge of the moment. At about the same time, I read enviously that the Japanese government, behaving more like Fineberg’s unified command, was distributing two reusable cloth face masks to every household because drugstores and shops had run out of supplies. We got our own first masks not from any U.S. source but from a Chinese colleague who had obtained extras from overseas relatives.
In its comprehensive estimates of national capacities, the GHSI also acknowledges a central role for politics, so central evidently as to remain unexplored and unquestioned. The executive summary notes: “Knowing the risks, however, is not enough. Political will is needed to protect people from the consequences of epidemics, to take action to save lives, and to build a safer and more secure world.” But whose political will, how activated, and how incorporated into the model? One may ask how a model of national capabilities built mainly on measurable indicators of health security was intended to account for such an intangible and volatile concept. Indeed, there is little evidence that the GHSI model incorporated variables such as federalism, political polarization and trust, income inequality, racial disparities, or marginalization of groups and regions in its calculations of preparedness. More foundationally, the GHSI assumed that all nations agree it is in their collective best interest to act in unison in a pandemic. Sadly, the chronicle of COVID-19—from the still unresolved question of how the virus first infected humans, to the surprising persistence of vaccine hesitancy—contradicts that basic assumption.
The playbook offers the most explicit statement of the political preconditions that would make its approach work. The domestic rubric, for instance, begins sensibly enough with the observation that, early in the trajectory of emergence, more will be unknown than known, and decisionmakers will have to act on incomplete information. Most of the succeeding assumptions, however, were based on ideals of ordered democracy dating from a less divisive time. They were quickly upended by unfolding events, positioning the United States as a “chaos country” in a comparative study I helped conduct during 2020. Notably, the U.S. government did not use all powers at its disposal to slow and mitigate the spread of disease, the National Security Council did not play the prescribed coordinating role, and states continued to wield a determining hand in policy, belying the expectation that the public would turn to the U.S. government for a concerted response.
It may be tempting to rejoin that human minds are fallible, and prediction and preparedness are at best guidelines for systematic analysis, not prescriptions for failsafe action. One might also argue that careful attention to the playbook’s checklist approach might have prevented embarrassing slip-ups such as the French government being unaware in its early modeling exercises that there were direct flights between Paris and Wuhan, the pandemic’s ground zero. But in fact the playbook and the Fineberg editorial have very much the look of blueprints, and the GHSI was less a map of the terrain than a guide to action: to “spur measurable changes in national health security and improve international capability” to address the “omnipresent risks” of a pandemic. Nor is the mismatch between expectation and performance limited to this pandemic alone. Our persistent failure to be prepared in times of crisis calls for another mindset, coupled to a deeper sensitivity toward the moral consequences of not knowing.
Technologies of Humility
Preparedness today is chain-linked to the power of computing. With massive advances in data science and technology, humankind is in a position to process information about almost anything that moves on the planet at sweeping scales and speeds. Capability feeds ambition. From climate change to consumer choice, we have grown used to the power of prediction, thereby imputing a presumption of regularity and a capacity for control to every aspect of human affairs.
The shocks of our era should remind us that such Promethean dreams need to be curbed by the limits of prediction. To be sure, technologists of preparedness may object that such awareness is already built into their methods. Garbage in, garbage out, as the computer scientists put it: everyone knows that bad inputs produce flawed outputs, and predictions are only as good as the data they rest on. Yet, too often imperfection is imagined only as a matter of defective data and erroneous calculation. From this vantage point, the chief lesson of failure is to get more data, improve the models, and do the same thing, only better, next time. The ethics and politics of prediction pass unnoticed, though if we care about the consequences of our action or inaction, these are the dimensions that should concern us most.
A Schmidt Futures Forum on Preparedness convened in January 2021 offered striking examples of such epistemic narrowing. Fineberg offered a brief keynote in which he extolled the value of science for policy but noted the need for a “high level of humility” in the face of what is not known and the diversity of possible viewpoints. He then joined a panel of four distinguished international public servants who addressed the mistakes and failings of science and science advice during the first year of the pandemic. Former U.S. Navy undersecretary Richard Danzig introduced the panel by echoing Fineberg’s appeal to humility and urged the guests to consider whether science had failed to account adequately for the vagaries of human behavior. In response, Margaret Hamburg, former FDA commissioner and a founder of the Nuclear Threat Initiative, revealed her continued allegiance to the preparedness paradigm, in which pandemics are primarily biological and actions fail mainly because science didn’t try to know soon enough what we all know we should have known. Citing virus variants, immune responses, and asymptomatic carriage as primary examples, Hamburg spoke about “efforts to identify critical gaps in knowledge that would affect the contours and control measures for this pandemic.”
In terms of the epistemic typology that Donald Rumsfeld made famous, Hamburg’s emphasis was on known unknowns, the problems that science should have more aggressively pursued. But precaution, as a foil to preparedness, invites us to reflect with humility on the unknown unknowns, the surprises lurking beyond the imaginations of the best-trained minds that end up hurting those least able to defend themselves. How can we cultivate a systematic mindset with respect to those dangers, and can we turn humility itself into a template for more robust collective action?
If there is one lesson to draw from the recurrent crises of preparedness, it is that non-knowledge does not absolve us of responsibility for the human tragedies created by our ignorance and error. Those are the problems that the technologies of humility are specifically geared toward addressing.
The starting point for any such exercise is to be sure we are asking the best questions. Has the problem been framed in the right way? From whose viewpoints is it being observed? And are we missing a forest of non-knowing for the sparse trees of scientific knowns? In the context of a pandemic, it could well be that too rigid a focus on fighting the disease agent, the primary concern of public health experts, causes us to miss other dimensions of wider moral concern, including questions of who is most likely to be infected or die if we do not get the infection under control. In seeking to act, did we consider who was most vulnerable and how the risks would be distributed? And if not, why not?
It’s not as if we could not have known. Given prior experience with health outcomes in the United States, it was not surprising that COVID-19 disproportionately affected the poor, the elderly, Blacks and Hispanics, and those living in environmentally compromised surroundings. Nor was it a shock that the dissolution of public service infrastructures—schooling, most notably—disproportionately affected women, single parents, and low-income families. Last but not least, members of these very underserved communities also proved to be most distrustful of the solutions science ultimately offered, including vaccines thrust upon groups that had historically and with good cause regarded organized medicine as their enemy. But as the GHSI, playbook, and Fineberg plan illustrate, social, political, and ethical concerns were not built into the tick boxes for what to ask and how to act that planners laid out before the pandemic escalated.
Had technologies of humility been more actively integrated into our schemes of governance and planning, we would not have missed phenomena such as vaccine hesitancy until they arrived on our doorstep as if unannounced. Where prediction runs the present out into the future, humility reverses time’s arrow and pulls possible futures back to show us how to act in the present. Humility’s concern is with consequences, but with special attention to the consequences of getting things wrong, leaving important viewpoints out, ignoring signs from the shadows in the certainty of having seen the light. Vaccine anxiety, after all, had been brewing for years around childhood immunization. Instead of dismissing these fears as illiterate and unscientific, and now paying the price, the technologies of humility would have asked, as some ethnographers did, why people did not trust the experts when their children’s health was at stake. That inquiry would have generated a map of power and powerlessness, and of resistance at the margins, that might have informed public policy very differently. It might have queried how, precisely, to implement Fineberg’s fifth injunction, to “inspire and mobilize the public.” Which public, and mobilize to what ends?
There is one respect in which the technologies of humility may be less humble than the techniques of prediction. When accidents and disasters happen, policymakers often dismiss them as unintended consequences, when in fact they were merely unforeseen by those with the capacity to act. Humility rejects this easy way out. It demands that we ask in advance what new vulnerabilities might be produced by our bravest acts of preparedness, in theaters of public health, economy, environment, or war. The technologies of humility would have us reflect longer and harder on the obligations we incur when acting on imperfect knowledge, by adopting the perspectives of those who are acted upon or are themselves not able to intervene. This is the cry of Lear on the heath when, stripped down to life’s bare essentials, he sees that he would have been a better king had he exposed himself “to feel what wretches feel.” Humility demands just that kind of self-abnegation from power and policy: to win greater knowledge because it sees from the margins as well as the center, and deeper wisdom because it acknowledges the imperfections of human understanding.
Boston Review is nonprofit and relies on reader funding. To support work like this, please donate here.