In the early 1930s two thousand predominantly Black workers were sent to tunnel through a mountain in Gauley Bridge, West Virginia. The mountain was made of silica, a crystalline compound in rock and sand that is toxic to the lungs. As historians David Rosner and Gerald Markowitz recount in Deadly Dust: Silicosis and the Politics of Occupational Disease in Twentieth-Century America (1991), the company was aware of these facts but sent the men to blast and dig the tunnel anyway, without safety precautions. The result was a massacre: the men inhaled the mineral dusts as they moved through the mountain, and as many as 1,500 of them acquired the lung disease silicosis, asphyxiating them in the coming months and years.
What explains respiratory inequities across race? Medical communities continue to point reflexively to nature rather than to society.
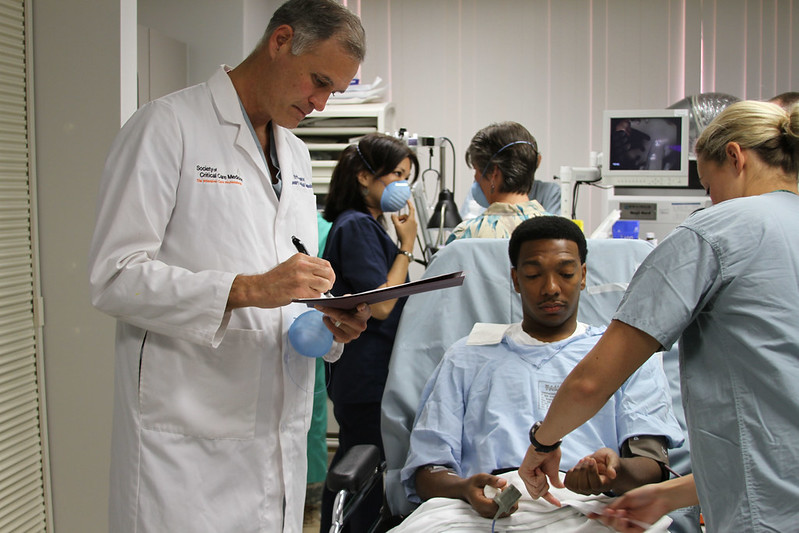
Almost a century later, Black men and women are still telling us they can’t breathe. Those words became famous in 2014 when New York City police killed Eric Garner in a chokehold. They provoked massive protests again this year when George Floyd uttered them shortly before being killed by Minneapolis police—in the midst of a pandemic of a debilitating respiratory disease that disproportionately afflicts Black communities. And even now, rates of death from silicosis are higher for Black men than white men. The thread connecting these respiratory deaths is not merely symbolic. The hierarchies that structure our society distribute not just wealth but breath.
Before COVID-19, asthma was the lung disease perhaps most closely associated with racial inequality. Black people are more likely than white people to have asthma and to die of it. Black children are less likely to be prescribed inhalers that control asthma and more likely to wind up in the emergency room unable to breathe. Influenza epidemics also disproportionately sicken the lungs of Black people: the 2009 H1N1 pandemic led to more hospitalizations among Blacks (and other non-white groups) than whites—indeed, more than double in the early wave. Black patients are also more apt to be hospitalized for pneumonia relative to whites, and among those hospitalized, more likely to die.
COVID-19 has been no exception to these trends. Early in the outbreak, reports from some localities suggested that Black people were disproportionately succumbing to the virus. A subsequent study in Health Affairs found that about one in four Black patients diagnosed with COVID-19 in a large California health system wound up in the intensive care unit, more than twice the rate among whites diagnosed with COVID-19. An investigation in the New England Journal of Medicine similarly revealed that while Black patients constitute about a third of the population of a large health system in Louisiana, they made up 71 percent of those hospitalized and 77 percent of those who died.
Just because diseases are ultimately biological phenomena does not mean they are not caused by social conditions.
What explains these respiratory inequities? Despite decades of important research on the social determinants of health, medical communities continue to point reflexively to nature rather than to society—to lungs being born this way rather than made this way. These accounts grossly understate the impact of structural oppression on respiratory outcomes. The lungs are the only vital organ in direct and continuous contact with our environment; it should not surprise us that they bear witness to our racialized geography. It is long past time for a reckoning with the ways repression impedes respiration.
• • •
The contention that Black lungs are intrinsically different than white lungs stretches back to our nation’s founding. As historian Lundy Braun describes in her seminal study Breathing Race Into the Machine: The Surprising Career of the Spirometer from Plantation to Genetics (2014), Thomas Jefferson’s Notes on the State of Virginia (1785) pointed to a “difference of structure in the pulmonary apparatus” as evidence of the suitability of Black people for plantation labor. Braun also examines explanations for the long-documented lower average lung function—measured as the volume of air a person can blow into a device called a spirometer—among Blacks relative to whites. Since the nineteenth century, Braun details, the medical profession has generally attributed these respiratory gaps to innate differences rather than to social inequality. More recently, a great deal of well-meaning medical research has been carried out in the shadow of these efforts, seeking genetic causes for higher rates of common diseases (including asthma) among Black people.
These explanations miss the way social conditions contribute to respiratory outcomes. DNA does not explain the blithe asphyxiation of Floyd, of course. As for asthmatics, there is no gene for being uninsured or underinsured: it is our corporatized, profit-oriented health financing system that forces those who suffer from asthma to go without needed medications or doctors’ visits because of cost. Nor is it ancestry that makes air pollution predominant in poor neighborhoods rather than rich ones. And the victims of the Gauley Bridge disaster did not have a genetic predisposition to silicosis; they were non-unionized workers who lacked collective power and whose corporate employer saw them as dispensable tools. (Black people are not the only such workers—other occupational lung diseases such black lung and asbestosis affect whites at higher rates than Blacks, in part due to worker demographics in Appalachia, where such diseases are particularly common—but Blackness makes it all the easier for workers to be marginalized in this way.)
The lungs are the only vital organ in direct and continuous contact with our environment; it should not surprise us that they bear witness to our racialized geography.
A growing body of work helps to correct the field’s neglect of the social determinants of health. As colleagues and I recently described in STAT, disparate exposure to pollutants, along with other forms of disadvantage, may help explain well-documented racial discrepancies in lung function. After all, striking differences in lung function—a strong predictor of life expectancy—are evident not only along racial lines but across class divisions. (As Braun notes, even the man credited with inventing the spirometer in the nineteenth century, the surgeon John Hutchinson, noted differences in average lung function among workers in different occupations.) Research in recent decades has also demonstrated, with striking consistency, that lung function slopes upward in a continuous gradient with rising education, income, and wealth. Socioeconomic disparities in lung function have been demonstrated throughout many time periods and across very different environments—from Shanghai to the Netherlands, Mexico, and Norway. It is likely that a slew of interconnected factors—including occupational exposures, indoor and outdoor air pollution, nutrition, lung infections, and likely much else—contribute to these inequities. There is some, albeit more limited evidence that psychosocial stress increases predisposition to the effects of air pollution, potentially leading to inflammation in the lungs that could contribute to worse outcomes.
One reason for confusion on these matters is that epidemiological studies have also found that differences in socioeconomic status (SES) do not “explain” the difference in lung function between whites and Blacks or play only a small role. But we must not interpret these results too hastily. It is highly implausible that the effects of racist exclusion in U.S. society can be captured by a simple statistical adjustment for income or education. For one thing, such measures typically do not account for stress, struggle, and exposure over the course of one’s life: just because someone happens to live in a middle-class neighborhood or have a relatively higher level of income now does not mean they always did. Residential redlining, wealth inequality, and structural segregation—things that explain, among other things, racially disparate exposure to diesel exhaust fumes—cannot be controlled for by a point-in-time measure of current family income or educational attainment.
Racial and economic oppression may also help to explain the disparate impact of the coronavirus pandemic within Black communities. A commonly cited potential mechanism for this disparity are comorbidities of chronic disease—e.g. heart disease or kidney failure—that confer increased risk for severe COVID-19, and which are indeed more common among Black people. But this does not mean Black people are naturally predisposed to those comorbidities, of course; racist exclusion almost surely plays a role in explaining disparate rates of chronic disease. While the precise physiological pathways have not been fully delineated, there is mounting evidence that adversity, material deprivation, and chronic psychosocial stress can be biologically toxic throughout one’s life, and that in some combination these conditions produce racial and class divides in metrics of health like blood pressure and kidney function as well as lung function.
But these comorbidities cannot be the only factor at work. While they may (in part) help explain worse outcomes among those infected, they fail to explain differing propensities to be infected at all. Given such higher rates of infection, it is not surprising that individuals of minority race and ethnicity, and of lower socioeconomic status, have a higher risk of COVID-19 mortality even when accounting for differences in chronic disease prevalence. One key factor may be, once again, occupational exposure. Black and Hispanic workers are more likely to be considered “essential,” or to work in jobs that afford less freedom to work from home, increasing exposure to the virus. Household crowding—a likely risk factor for dissemination within the home—could also be a factor: a recent study by colleagues found that some 81 million people—disproportionately lower income, Hispanic, Black, and Native Americans—live in homes without enough space or plumbing to allow family members to isolate were one to be infected.
Another important social factor to consider is inequitable access to health care. Those who are at increased risk of severe COVID-19 due to comorbidity are also less likely to have adequate health care. Our recent study found that some 18 million Americans who are at increased risk of severe COVID-19 due to advanced age or chronic illness—disproportionately racial and ethnic minorities and those with low incomes—are either uninsured or underinsured. Another study I recently published with colleagues, based on an analysis on national survey data, found that 29.2 percent of individuals out sick from work with symptoms they attributed to the coronavirus were uninsured—far higher than the rate for the overall population. We know that cost concerns cause those in the throes of a heart attack to delay medical care. We don’t know whether this is true for COVID-19, too—and with what consequences—but one national poll did find that some 9 percent of individuals with symptoms they believed were due to COVID-19 would avoid treatment because of cost. The rate, unsurprisingly, was higher among non-whites and those with lower incomes.
Air pollution, stress, occupational hazards, and health care services are distributed, unequally, across the intertwined divides of class and race.
These deficiencies lead to racial and socioeconomic inequities in the “effective demand” for health care, producing a distorted distribution of the utilization of care. But inequities in supply are no less important. Health care infrastructure in the United States is shaped by market mechanisms that have yielded a gross geographic maldistribution of resources. An April study in the Journal of the American Medical Association, for instance, found that the number of COVID-19 hospitalizations and deaths was highest in the Bronx and lowest in Manhattan, yet Manhattan has more than 50 percent more beds per capita than the Bronx. Nationwide, the regional distribution of ICU beds depends, in part, on a community’s income: about half of areas with a low median income are without a single ICU bed, whereas only 3 percent of high-income communities lack critical care beds. These sorts of maldistributions are manifestations of what the British GP and epidemiologist Julian Tudor Hart famously called the “Inverse Care Law”: those areas most in need of medical care tend to be those where it is least available. The law is most in force, Hart emphasized, where market mechanisms predominate. We need a health system where medical infrastructure and resources are not distributed according to the dictates of the market, but rationally planned according to community health needs.
On top of all these social factors, there are also “intrinsic” biases among health care workers themselves. These are no doubt a problem, too, though there is at least some evidence that “single-tier” health systems make a difference. A study of some six million individuals in the Veterans Affairs (VA) health system, for instance, found that while Black and Hispanic individuals were more likely to be diagnosed with COVID-19, there were no differences in outcomes among those infected. This research tracks with a broader body of evidence that ubiquitous racial divides in health outcomes in the United States are substantially attenuated in the VA.
• • •
Mechanisms matter. As historian Merlin Chowkwanyun and political scientist Adolph L. Reed, Jr., argued in the New England Journal of Medicine in July, reciting “disparity figures without explanatory context can perpetuate harmful myths and misunderstanding that actually undermine the goal of eliminating health inequities”—by reifying race as biology, for example, or perpetrating the stigmatization of certain communities.
The hierarchies that structure our society distribute not just wealth but breath. It is long past time for a reckoning with the ways repression impedes respiration.
At the same time, we have to recognize that mechanisms themselves often reflect social inequities. Just because diseases are ultimately biological phenomena does not mean they are not caused by social conditions. Air pollution, stress, occupational hazards, and health care services are distributed, unequally, across the intertwined divides of class and race. Even as health hazards and salubrious resources have changed over the centuries—as air quality worsened and improved, as medical care went from being mostly useless to often lifesaving, as mining and manufacturing collapsed while the service economy swelled—the fundamental link between race, class, and health has persisted. This is what public health scholars Bruce Link and Jo Phelan meant when they argued in a highly influential article in 1995 that socioeconomic factors should be deemed “fundamental causes of disease.”
We need more of that thinking today. In the wake of the events this year, there appears to be growing recognition within medical communities that racism is a public health problem. In order to take advantage of that mounting awareness, we must emphasize that it is a problem that can be solved only by confronting the structural economic inequities that distribute, among other things, the means of good pulmonary health.